Time to Talk Day, is observed on 5th February 2026, and serves as a pivotal reminder of the importance of open dialogues in addressing mental health issues across the UK. As the nation’s largest annual mental health conversation event, it encourages individuals, communities, and workplaces to discuss wellbeing without stigma.

This article explores its history and premise, provides a comprehensive list of UK support groups, highlights the pressing concerns around male mental health and suicide rates, and examines the efficacy of talking therapies; including potential iatrogenic harms. My aim is to offer a balanced, evidence-based perspective.
History and Premise of Time to Talk Day

Time to Talk Day was launched on the 6th February 2014, as part of the “Time to Change” campaign, a collaborative initiative by mental health charities Mind and Rethink Mental Illness, it was, and is, funded by organisations such as Comic Relief and the Department of Health and Social Care. The premise centres on normalising conversations about mental health to reduce stigma, improve support networks, and encourage behaviours that seek help, instead of staying silent and struggling alone. It is held on the first Thursday in February each year, promoting activities like ‘Tea and Talk’ sessions or social media sharing under #TimeToTalkDay.
The campaign’s roots trace back to broader efforts to combat mental health discrimination, with partnerships expanding over time, such as with the Co-op in 2022 to enhance community outreach. Although Time to Change concluded in 2021, Mind and Rethink Mental Illness pledged to sustain the day, focusing on themes like therapy access and support in the aftermath of a suicide attempt; for those who have attempted suicide themselves (e.g., coping with overwhelming emotions and navigating next steps) and for friends, family, or others providing support to attempt survivors.

Its growth into a global movement underscores the premise that simple talks can mitigate isolation, enhance mood, and foster resilience, building on historical concepts like Freud’s ‘talking cure’ from the 1890s.
UK Support Groups for Mental Health
The UK boasts a wide array of support groups and charities dedicated to mental health, offering peer support, helplines, and specialised services. Below is a comprehensive list compiled from multiple sources, focusing on national organisations. Local branches can often be found via tools like the Hub of Hope database.
This list is not exhaustive but represents key players across various needs.
Organisations
- Mind: General mental health support, including local Minds for peer groups and advocacy. Website: www.mind.org.uk; Helpline: 0300 123 3393
- Rethink Mental Illness: Support for severe mental illness, with over 150 peer groups in England. Website: www.rethink.org; Advice Line: 0808 801 0525
- Samaritans: 24/7 emotional support for anyone in distress. Website: www.samaritans.org; Helpline: 116 123
- Mental Health Foundation: Information and resources on prevention and wellbeing. Website: www.mentalhealth.org.uk
- SANE: Emotional support for those affected by mental illness. Website: www.sane.org.uk; Helpline: 0300 304 7000
- Campaign Against Living Miserably (CALM): Suicide prevention, particularly for men, with focus on stigma reduction and support for those in crisis. Website: www.thecalmzone.net; Helpline: 0800 58 58 58 (5pm-midnight, 365 days a year)
- Anxiety UK: Support for anxiety conditions. Website: www.anxietyuk.org.uk; Helpline: 03444 775 774
- Bipolar UK: Peer support for bipolar disorder. Website: www.bipolaruk.org.uk
- Hub of Hope (Chasing the Stigma): National directory of mental health services. Website: hubofhope.co.uk
- National Survivor User Network (NSUN): Peer support for survivors of mental health services. Website: www.nsun.org.uk
- Op COURAGE (NHS Veterans’ Mental Health and Wellbeing Service): Specialist NHS service for veterans, reservists, and service leavers, including mental health assessments and treatments. Website: www.nhs.uk/nhs-services/armed-forces-community/mental-health/veterans-reservists; Self-referral available
- Together UK: Community-based support groups. Website: www.together-uk.org
- Mental Health Mates: Walking groups for mental health. Website: www.mentalhealthmates.co.uk
- Student Minds: University-focused peer support. Website: www.studentminds.org.uk
- Relate: Relationship counselling impacting mental health. Website: www.relate.org.uk; Helpline: 0300 100 1234
- British Association for Counselling and Psychotherapy (BACP): Directory for therapists and support. Website: www.bacp.co.uk
- Andy’s Man Club: Free peer-to-peer support groups for men, aimed at suicide prevention and open conversations. Website: www.andysmanclub.co.uk; Groups nationwide, every Monday 7pm (except bank holidays)
- Men’s Sheds UK: Community workshops and spaces for men to connect, reduce isolation, and engage in practical activities. Website: www.menssheds.org.uk; Local sheds across the UK
- ManHealth: Peer support networks for men experiencing mental health difficulties, particularly in northern England. Website: www.manhealth.org.uk; Support groups and online resources
- HUMEN: Anonymous, non-clinical support meetings for men to discuss mental health and wellbeing. Website: www.wearehumen.org; Free sessions across the UK
- Combat Stress: Dedicated mental health support for veterans with complex issues like PTSD, anxiety, and depression. Website: www.combatstress.org.uk; Helpline: 0800 138 1619 (24/7)
- Help for Heroes (Hidden Wounds): Mental health therapy and wellbeing support for veterans and their families, including CBT and counselling. Website: www.helpforheroes.org.uk; Self-referral via online form
- Walking With The Wounded (Head Start): Access to private therapy for veterans dealing with mental health issues like PTSD and adjustment disorder. Website: www.walkingwiththewounded.org.uk; Partnerships with NHS and therapists
- PTSD Resolution: Short-term counselling for veterans experiencing trauma-related mental health problems. Website: www.ptsdresolution.org; Free services for veterans
- SSAFA (Soldiers, Sailors, Airmen and Families Association): Support for serving and veteran armed forces personnel and families, including mental health guidance and referrals. Website: www.ssafa.org.uk; Helpline: 0800 260 6767
- Royal British Legion: Comprehensive support for veterans, including mental health advice, financial aid, and community services. Website: www.britishlegion.org.uk; Helpline: 0808 802 8080
- Carers UK: Support for carers affected by mental health issues. Website: www.carersuk.org; Helpline: 0808 808 7777
These groups provide empathy, information, and community, often run by volunteers with lived experience. For crisis support, always contact Samaritans, NHS 111 or emergency services (999).
The Crisis in Male Mental Health and Suicide Rates: Insights from Dr John Barry
Male mental health remains a critical concern in the UK, where men account for three-quarters of suicides, with rates peaking among those aged 40-54. Dr John Barry, a chartered psychologist, researcher, author, clinical hypnotherapist, and co-founder of the Centre for Male Psychology (@CentreMalePsych), has been instrumental in highlighting these issues.

His work emphasises that men often experience mental health differently, with symptoms like irritability or substance misuse rather than overt sadness, leading to underdiagnosis. Barry’s research, including contributions to the Palgrave Handbook of Male Psychology and Mental Health (2019) and Perspectives in Male Psychology (2021), points to factors such as economic adversity, relationship breakdowns, and barriers to seeking help or support. He advocates for male-friendly therapies, noting that traditional approaches may overlook male-specific needs, exacerbating issues like homelessness and addiction.
Recent data from 2010-2021 shows only 37.3% of male youth suicides had a prior mental health diagnosis, underscoring gaps in recognition and support. Dr Barry frequently address these, promoting initiatives like suicide prevention standards and empathetic help-seeking narratives.
The Efficacy of Talking Therapies: Benefits and Potential Harms
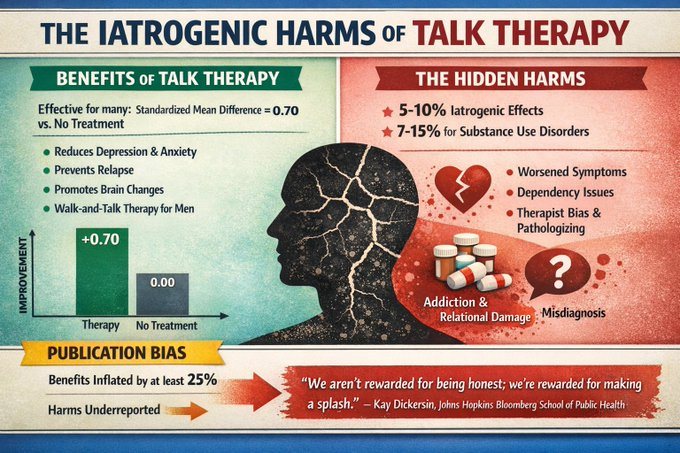
Evidence reveals that talking therapies, such as cognitive behavioural therapy (CBT) and psychotherapy, can be effective for many, with standardised mean differences around 0.70 compared to no treatment, particularly for depression and anxiety. They can reduce symptoms, prevent relapses, and promote long-term brain changes, often matching or surpassing medication efficacy. For men, walk-and-talk variants show promise in engagement and distress reduction.
However, iatrogenic harms, unintended negative effects, affect around 5-10% of cases, with higher rates (7-15%) for substance use disorders, including worsened symptoms, dependency, or relational damage from pathologising normal emotions or therapist biases. Publication bias may overstate benefits by at least 25%, and harms like emotional escalation or misdiagnosis are under-researched. Of course, publication bias isn’t limited to depression treatments. It’s a widespread problem throughout the research world, says Kay Dickersin, a professor of epidemiology at Johns Hopkins Bloomberg School of Public Health.
“We’re rewarded for getting papers out, for finding results that will bring attention to our universities and to ourselves,” she says. “We aren’t rewarded for being honest; we’re rewarded for making a splash.”
Personal Reflections on Talk Therapy
I must express a degree of scepticism regarding talk therapy, given the documented iatrogenic harms. Instances where therapy pathologises everyday emotions or fosters dependency can exacerbate issues rather than resolve them, potentially leading to long-term distrust or worsened mental states. That said, if it resonates with an individual, and for them yields positive outcomes; such as reduced anxiety or improved coping strategies, then pursuing it is worthwhile. If harms emerge, seeking alternatives like peer support, exercise, or male-tailored approaches may prove more beneficial.
Conclusion
Time to Talk Day embodies the power of conversation in mental health, yet broader challenges like male suicide rates and therapy harms demand nuanced approaches. By leveraging support groups and evidence-based insights, we can foster genuine progress. So if it works as a first step, or a step that leads you to reduced stigma, then let’s get talking!
References
- Westra, H.A. (n.d.) ‘Does Therapy Work? Evaluating Its Effectiveness and Benefits’. Available at: https://therapygroupdc.com/therapist-dc-blog/does-therapy-work-evaluating-its-effectiveness-and-benefits (Accessed: 5 February 2026).
- American Psychological Association (2012) Understanding psychotherapy and how it works. Available at: https://www.apa.org/topics/psychotherapy/understanding (Accessed: 5 February 2026).
- Barry, J. (2019) Psychological aspects of polycystic ovary syndrome. Palgrave Macmillan.Barry, J. and Liddon, L. (2021) Perspectives in male psychology: an introduction. Wiley. https://thecentreformalepsychology.thinkific.com/courses/IntroductiontoMalePsychologyandMentalHealth (Accessed: 5 February 2026).
- Boisvert, C.M. and Faust, D. (2002) ‘Iatrogenic symptoms in psychotherapy: a theoretical exploration’, American Journal of Psychotherapy, 56(2), pp. 244-259.
- British Psychological Society (2022) Psychological interventions to help male adults. BPS.
- Centre for Male Psychology (2024) World Suicide Prevention Day 2020: another day, another deaf ear for men. Available at: https://www.centreformalepsychology.com/male-psychology-magazine-listings/world-suicide-prevention-day-2020-another-day-another-deaf-ear-for-men (Accessed: 5 February 2026).
- Cuijpers, P. et al. (2019) ‘Is psychotherapy effective? A re-analysis of treatments for depression’, Epidemiology and Psychiatric Sciences, 28(3), pp. 268-274.
- Daysoftheyear.com (2024) Time to Talk Day (February 5th, 2026). Available at: https://www.daysoftheyear.com/days/time-to-talk-day (Accessed: 5 February 2026).
- Education Support (2024) Time to Talk Day. Available at: https://www.educationsupport.org.uk/resources/for-individuals/articles/time-to-talk-day (Accessed: 5 February 2026).
- Eysenck, H.J. (1978) ‘An exercise in mega-silliness’, American Psychologist, 33(5), pp. 517.
- First Response Training (2025) Time to Talk Day 2025: the nation’s biggest mental health conversation. Available at: https://www.firstresponsetraining.com/time-to-talk-day-2025-the-nations-biggest-mental-health-conversation (Accessed: 5 February 2026).
- Fountain, J. et al. (2024) ‘Suicide by middle-aged men’, National Confidential Inquiry into Suicide and Safety in Mental Health. Available at: https://sppcm.co.uk/wp-content/uploads/2024/10/NCISH_2021-Suicide-by-middle-aged-men-report.pdf (Accessed: 5 February 2026).
- Gorman, J.M. and Gorman, J.M. (2018) ‘The science of psychotherapy’, Dialogues in Clinical Neuroscience, 20(3), pp. 175-182.
- HCPC Careers (2024) Revealing the Heartfelt Conversations: Our Reflections on Time to Talk Day. Available at: https://www.careers.hcpc-uk.org/blog/2024/02/revealing-the-heartfelt-conversations-our-reflections-on-time-to-talk-day (Accessed: 5 February 2026).
- Heartwise Support (2025) The Power of Talk Therapy in Mental Health Healing. Available at: https://www.heartwisesupport.org/post/power-of-talk-therapy-in-mental-health-healing (Accessed: 5 February 2026).
- Hollon, S.D. et al. (2015) ‘Studies May Overstate The Benefits of Talk Therapy For Depression’, NPR. Available at: https://www.npr.org/sections/health-shots/2015/09/30/444789771/studies-may-overstate-the-benefits-of-talk-therapy-for-depression (Accessed: 5 February 2026).
- Howard, K.I. et al. (1986) ‘The dose-effect relationship in psychotherapy’, American Psychologist, 41(2), pp. 159-164.
- Inspire Wellbeing (2024) Time to Talk Day. Available at: https://www.inspirewellbeing.org/time-to-talk-day (Accessed: 5 February 2026).
- Levy, K.N. and Ablon, J.S. (2010) ‘Change in psychotherapy: a plea for greater integration’, American Journal of Psychiatry, 167(8), pp. 886-888.
- Lilienfeld, S.O. (2007) ‘Psychological treatments that cause harm’, Perspectives on Psychological Science, 2(1), pp. 53-70.
- Malhotra, A. and Sahoo, S. (2017) ‘Rebuilding the brain with psychotherapy’, Indian Journal of Psychiatry, 59(4), pp. 411-419.
- Mason, L. et al. (2017) ‘Brain connectivity changes occurring following cognitive behavioural therapy for psychosis predict long-term recovery’, Translational Psychiatry, 7(1), p. e1001.
- Mental Health America (2024) Science Behind Therapy. Available at: https://mhanational.org/resources/science-behind-therapy (Accessed: 5 February 2026).
- Mind (2024a) How to find a support group. Available at: https://www.mind.org.uk/information-support/guides-to-support-and-services/peer-support-groups/how-to-find-a-support-group (Accessed: 5 February 2026).
- Mind (2024b) Time to Talk Day. Available at: https://www.mind.org.uk/get-involved/time-to-talk-day (Accessed: 5 February 2026).
- Mind (2024c) We’re Mind, the mental health charity. Available at: https://www.mind.org.uk/ (Accessed: 5 February 2026).
- NHS (2024) Support groups – Depression in adults. Available at: https://www.nhs.uk/mental-health/conditions/depression-in-adults/support-groups (Accessed: 5 February 2026).
- Parry, G.D. et al. (2016) ‘Iatrogenic harm from psychological therapies–time to move on’, British Journal of Psychiatry, 208(3), pp. 210-212.
- Rethink Mental Illness (2024) Our peer support groups. Available at: https://www.rethink.org/help-in-your-area/support-groups (Accessed: 5 February 2026).
- Safe New Futures (2024) What is ‘Time to Talk Day’?. Available at: https://www.safe.org.uk/2024/01/31/what-is-time-to-talk-day (Accessed: 5 February 2026).
- Seager, M. et al. (2016) ‘The male gender empathy gap: time for psychology to take action’, New Male Studies, 5(1), pp. 6-16.
- Shedler, J. (2010) ‘The efficacy of psychodynamic psychotherapy’, American Psychologist, 65(2), pp. 98-109.
- Smith, M.L. and Glass, G.V. (1977) ‘Meta-analysis of psychotherapy outcome studies’, American Psychologist, 32(9), pp. 752-760.
- Time to Change (2016) It’s Time to Talk. Available at: https://epi.org.uk/publications-and-research/its-time-to-talk (Accessed: 5 February 2026).
- Time to Change (2024) Other useful organisations. Available at: https://www.time-to-change.org.uk/what-are-mental-health-problems/mental-health-help-you/other-useful-organisations (Accessed: 5 February 2026).
- Time to Change (n.d.) Summary of impact and learning. Available at: https://www.time-to-change.org.uk/sites/default/files/TTC_Phase2_legacy_Time_To_Talk_Day.pdf (Accessed: 5 February 2026).
- University College London (2021) Dr John Barry explores psychological aspects of men and boys in new book. Available at: https://www.ucl.ac.uk/brain-sciences/news/2021/apr/dr-john-barry-explores-psychological-aspects-men-and-boys-new-book (Accessed: 5 February 2026).
- Vulnerability Registration Service (2024) List of Mental Health Organisations in the UK. Available at: https://www.vulnerabilityregistrationservice.co.uk/mental-health-care-companies (Accessed: 5 February 2026).
- Wampold, B.E. and Imel, Z.E. (2015) The great psychotherapy debate: the evidence for what makes psychotherapy work. 2nd edn. Routledge.
- Westra, H.A. (n.d.) ‘Does Therapy Work? Evaluating Its Effectiveness and Benefits’. Available at: https://therapygroupdc.com/therapist-dc-blog/does-therapy-work-evaluating-its-effectiveness-and-benefits (Accessed: 5 February 2026).
