
The Green Party’s Radical Drug Legalisation Proposal For The UK: Ignoring Evidence of Harm and Global Policy Failures; An Introduction:
The Green Party’s manifesto push to legalise hard drugs like crack cocaine, heroin, GHB (gamma-hydroxybutyric acid), methamphetamine, for recreational use. This includes allowing high-street sales, availability in nightclubs, and even NHS prescriptions for substances like crack and methamphetamine, representing a dangerous detachment from reality. Proponents claim it promotes “freedom,” could dismantle criminal networks, and enhance “relationships and creativity” through “limited” use. However, this ignores decades of evidence showing the profound physical, mental, and societal harms these substances inflict, especially on young people already grappling with epidemics like ketamine abuse in the UK!

Drawing from medical research, epidemiological data, and real-world policy outcomes, this article dissects the severe risks of these drugs and examines why similar liberalisation efforts in places like Canada, Oregon, Portugal, the Netherlands, British Columbia, San Francisco, and Seattle have often led to increased use, overdoses, crime, and public disorder. Evidence shows that full legalisation or decriminalisation, amplifies problems rather than solving them. It also examines potential devastating impacts on UK society and the NHS, incorporates and refutes key counterarguments from pro-legalisation viewpoints and findings for a balanced evaluation and conclusion.
Legalisation/Decriminalisation Often Increases Drug Use and Harms
Other countries who have legalised drugs have seen drug use increase, especially for frequency and among adults. While decriminalisation (removing possession penalties) has mixed results, full legalisation (commercial sales like the Greens propose) tends to boost use, as seen with cannabis. For hard drugs, evidence suggests even bigger risks.
- Cannabis Legalisation in Canada and US States: Post-2018 legalisation in Canada, past-month adult use rose from 14% (2018) to 20% (2020), past-year use from 22% (2018) to 25% (2021), with the biggest jumps in 25-44-year-olds. Daily/near-daily use hit 6% by 2023 (up from 5% pre-legalisation). In US states, adult past-month use increased 26% post-legalisation (vs. non-legal states), frequent use 23%, and cannabis use disorder 37% among adults 26+. Non-college young adults (18-24) saw past-month use rise from 23% to 28%, frequent use from 12% to 14%. Overall US daily users now outnumber daily drinkers, with prevalence doubling since the 1980s. Emergency visits for cannabis rose in some states, tied to higher potency and edibles.
- Oregon’s Decriminalisation: Initial 2021 data showed 23% overdose increase (182 extra deaths), but later analyses controlling for fentanyl found no link; fentanyl drove the spike (overdoses up everywhere, Oregon’s rise similar to Washington’s). Crime and overdoses followed pre-pandemic trends/COVID/fentanyl, not necessarily tied to the change in law. However, Oregon re-criminalised drugs in 2024 amid public backlash.
- British Columbia’s Pilot: Led to a spike in hospitalisations. Public Backlash, associated with opioid hospitalisations up 58%; and open drug use led to recriminalisation.
- San Francisco and Seattle: Disorder and Overdoses soared and their Liberal policies led to open use, crime went up 33%, overdoses among homeless 24% of totals; due to this recriminalisation efforts are underway.
- Portugal’s Decriminalisation (Not Full Legalisation): Often cited as success, but it’s decriminalisation (no penalties for possession, but no commercial sales). Overdose deaths fell 80% (from 80/million in 2001 to 6/million in 2021), HIV from injections dropped 90%, treatment access up 60%. But lifetime use rose from 7.8% (2001) to 12.8% (2022), overdoses hit 12-year highs recently (doubled in Lisbon since 2019), crime up 14% (2021-2022). Not quite the utopia the Greens are implying; harms persist, and it’s not even full legalisation.
- Broader Evidence on Hard Drugs: Netherlands’ marijuana liberalisation doubled youth use, tripled heroin addiction. Legalising hard drugs like heroin/crack would spike use, and addiction (e.g., as it would be more accessible, cheaper), health costs, crime/violence. GHB (date-rape drug) risks misuse for assaults if sold openly. Partnerships with cartels? That empowers criminals, it does not dismantle them.
The Greens’ idea of teaching “safe” hard drug use in primary schools and cracking down on alcohol and tobacco instead is absurd. Alcohol and tobacco harms are huge because they’re legal and marketed. Adding crack, heroin, GHB to that mix would create more “drug-ridden” chaos, as Labour warns. Evidence shows liberalisation often increases use and harms, especially without strict controls the Greens downplay. This isn’t just “insane” it’s dangerously out of touch with reality.
Comprehensive List of Illegal Drugs in the UK and Their Classifications
Under the Misuse of Drugs Act 1971, illegal drugs are categorised into Classes A, B, and C based on perceived harm to users and society, with penalties escalating accordingly. Class A drugs are deemed most harmful, carrying up to life imprisonment for supply; Class B up to 14 years; Class C up to 2 years. These classifications guide enforcement but do not always align with scientific harm assessments, for example alcohol, which is legal, ranks higher in harm than some Class A drugs per multicriteria analyses. This proposal would legalise them all, amplifying risks.
Key illegal drugs include:
- Class A (Highest Harm): Includes crack cocaine, cocaine, ecstasy (MDMA), heroin, LSD, magic mushrooms (psilocybin), methadone, methamphetamine. These are highly addictive, with severe medical and social consequences.
- Class B (Moderate Harm): Amphetamines, cannabis, codeine, ketamine. Often stimulants or depressants with dependency risks
- Class C (Lower Harm): Anabolic steroids, benzodiazepines (e.g., diazepam), GHB. Includes performance enhancers and sedatives with misuse potential. The government has changed the law meaning it is now illegal to possess nitrous oxide to ‘get high’ with, making it a Class C drug.
Medical harms involve direct physical/mental health effects (e.g., organ damage, psychosis); social harms encompass broader impacts (e.g., crime, family breakdown, economic costs). Medical harms are individual (e.g., liver failure from heroin); social harms are communal (e.g., violence from drug markets). Illegal drugs cost UK society £20bn per year both medically and socially. The following sections detail harms for major drugs, focusing on long-term effects medically ad socially.
Detailed Harms of Major Drugs: Medical vs. Social Impacts
The Severe Risks of Crack Cocaine:
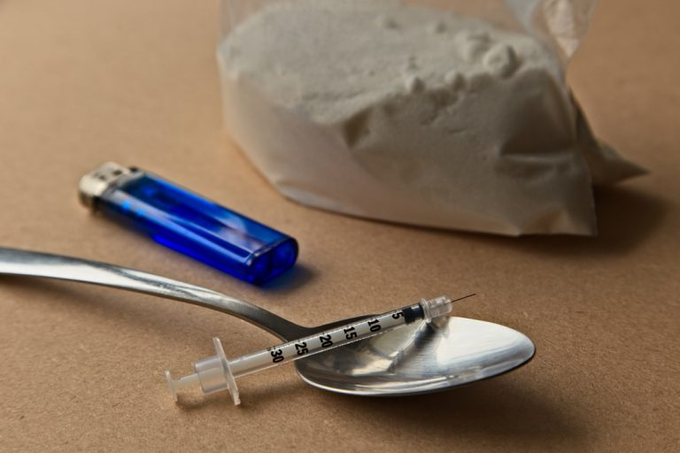
A Fast Track to Organ Failure and Mental Collapse; Intense Addiction and Societal Violence. Sometimes referred to as: Blow, C, Chang, Charlie, Ching, Coke, Crack, Flake, Freebase, Pebbles, Percy, Rocks, Sniff, Snow, Stones, Toot, Wash, or White, crack cocaine is a white or off-white rock-like substance. It takes its name from the characteristic cracking or popping noise it makes when it’s exposed to heat. When smoked, crack cocaine offers an intense feeling of euphoria. Crack cocaine is considered the most addictive form of cocaine, making it a highly dangerous substance. It delivers an intense but short-lived high, leading users to binge repeatedly. Long-term use wreaks havoc on the body and brain, often irreversibly. Public Health England estimates that there are over 180,000 users in the UK, a figure that risen significantly throughout the 2010s.

Chronic abuse causes cardiovascular damage, including elevated blood pressure, rapid heartbeat, and vasoconstriction, increasing risks of heart attacks, strokes, and sudden death; even in young, healthy individuals. Respiratory issues are rampant, especially from smoking, leading to lung damage, chronic bronchitis, and “crack lung”, a condition involving severe breathing difficulties and potential collapse. Users often suffer gastrointestinal problems like tears, ulcers, and severe weight loss due to suppressed appetite.
Crack reduces oxygen flow to the brain, causing damage that impairs memory, attention, and decision-making. Mental health deteriorates with chronic depression, anxiety, paranoia, psychosis, and hallucinations that can persist long after quitting. A users physical appearance suffers too: “meth mouth”-like tooth decay, skin sores, and accelerated aging. For young users, the risks are amplified, with higher chances of addiction and permanent cognitive deficits. Legalising sales would normalise this, likely spiking use and these lifelong harms.

This intense craving not only devastates physical health, but also fuels broader societal violence, as users and dealers engage in aggressive behaviours to sustain supply chains and territorial control.

- Powder cocaine, often perceived as a more “refined” or recreational stimulant compared to crack cocaine, exerts a subtle but cumulative destruction on users through prolonged exposure rather than the explosive, immediate grip of its smokable counterpart. While both derive from the same coca plant alkaloid and produce similar stimulant effects by blocking dopamine reuptake, the key distinction lies in the route of administration: powder cocaine is typically snorted (or occasionally injected), delivering a slower onset of euphoria that lasts 15–30 minutes, fostering patterns of sustained or binge use over time rather than frantic redosing.
- Medically, powder cocaine inflicts significant physical damage primarily through its method of use, such as severe nasal damage including perforated septum’s from chronic snorting, alongside broader cardiovascular risks like heart attacks, arrhythmias, strokes, and strain on the liver and kidneys from prolonged toxicity. Mentally, it contributes to long-term issues including depression, anxiety, paranoia, psychosis, memory impairment, and accelerated brain aging due to neurotoxic effects and disrupted dopamine pathways. Additional harms include impotence (from vascular damage) and malnutrition, as users often neglect nutrition amid sustained binges or financial strain. These effects build gradually, contrasting sharply with crack cocaine’s rapid, intense highs that drive acute paranoia, respiratory damage (“crack lung”), and immediate overdose risks, though both share overlapping cardiovascular and neurological dangers.
Socially: In the UK, crack cocaine’s grip has been linked to escalating conflicts within communities, where its distribution often intersects with organised crime networks.

- The social harms of crack cocaine extend deeply into crime, driving increases in theft and violence as addicts resort to desperate measures to fund their habits. Theft becomes a common survival tactic, with users stealing from homes, shops, or even family members to afford the next hit, contributing to a broader erosion of community trust and safety. Violence is equally pervasive, manifesting in assaults, robberies, and disputes over drug debts or territory, often exacerbated by the drug’s paranoia-inducing effects. In areas plagued by crack markets, such as major cities, this has led to heightened fear among residents and strained law enforcement resources, with drug-related offenses accounting for a significant portion of police workloads.
- Exploitation is another grim element of crack cocaine’s impact, particularly through the practice known as “cuckooing,” where drug dealers target and takeover the homes of vulnerable individuals to use as bases for storage, dealing, or production. Named after the cuckoo bird’s habit of invading nests, this form of criminal exploitation often preys on people with mental health issues, addictions, disabilities, or social isolation, coercing them through threats, debt bondage, or false promises of drugs or money. Victims may find their properties turned into hubs for illegal activities, leading to further victimisation, eviction risks, and entanglement in criminal proceedings if authorities discover drugs on the premises. This tactic is closely tied to county lines operations, where gangs expand their reach from cities to rural areas, amplifying exploitation across regions.

- Family breakdown is a profound consequence of crack cocaine addiction, tearing apart households through financial ruin, neglect, and emotional turmoil. Addicted parents may prioritise the drug over childcare, leading to child welfare interventions, domestic abuse, or the dissolution of relationships as trust erodes under the weight of lies and erratic or abusive behaviour. Children in these environments face heightened risks of trauma, poverty, and even recruitment into drug-related activities, perpetuating intergenerational cycles of harm. Support services report that family members often suffer secondary effects, such as mental health declines or isolation, as they grapple with enabling behaviours or failed attempts to help their loved ones.
- In the UK, crack cocaine affects over 180,000 users, with estimates from around 2015 placing the number at approximately 182,828 in England alone, though more recent figures suggest ongoing prevalence amid fluctuating trends. Treatment demand has risen notably, with a 19% increase in adults entering services for crack-related issues between 2015-16 and 2017-18, reflecting growing recognition of the problem despite barriers like stigma and limited access. By 2024-25, around 19% of new treatment entrants cited crack as a primary concern, totalling over 32,000 people, underscoring the drug’s persistent hold on vulnerable populations.
- Crack cocaine significantly contributes to societal violence, linked to roughly half of homicides in England through gang-related activities and drug market disputes. The drug’s markets are inherently volatile, with territorial rivalries and debt enforcement often escalating to lethal confrontations, including knife crime and shootings. Between 2014 and 2017, drug-related homicides rose from 50% to 57% of cases, driven by crack’s role in fuelling competition among dealers and organised crime groups. This violence not only claims lives but also perpetuates fear in communities, highlighting the urgent need for integrated approaches to disrupt supply chains and support recovery.
- Socially, high dependency on powder cocaine frequently results in financial ruin through escalating costs, often viewed as a “premium” drug, resulting in job loss as performance declines or erratic behaviour emerges over months or years. It links to various forms of crime, including fraud, embezzlement, or low-level dealing to sustain habits, as well as exploitation within supply chains, though less overtly violent than crack markets. Powder cocaine’s profile often aligns more with middle-class or nightlife scenes than the concentrated urban deprivation seen with crack. Overall, while crack cocaine’s harms manifest in explosive, immediate societal violence and rapid addiction spirals, powder cocaine’s damage accrues quietly yet relentlessly, eroding health, finances, and stability through sustained, often normalised consumption.
The Devastating Effects of Heroin: Profound Dependence and Health Devastation
Withdrawal is agonising, fuelling cycles of use and relapse. Legalisation could exacerbate access, mirroring cannabis trends where use rose post-legalisation, leading to more addiction and societal costs. In addition to previously stated social harms; in the section above: High addiction/withdrawal cycles with Heroin fuel crime (theft, dealing), family neglect, homelessness; There are approximately 300,000+ UK opiate/crack addicts, it contributes to £20bn in societal costs.
Heroin, an opioid derived from morphine, induces euphoria but rapidly leads to tolerance and dependence. A powerful opiate that’s usually sold as a white or brown powder. Also called: Brown, Gear, H, Horse, Skag, or Smack. Long-term use alters brain structure, causing neuronal imbalances that impair decision-making, stress response, and behaviour regulation. Users experience chronic depression, anxiety, psychosis, and cognitive decline, including memory loss and reduced learning ability. Physical tolls include liver, kidney, and lung diseases; collapsed veins; abscesses; and infections like HIV, hepatitis, and endocarditis from needle use. Young people are particularly vulnerable, with accelerated biological aging, telomere shortening (the progressive reduction in the length of protective DNA caps), and brain changes that heighten risks of coma, cognitive impairment, and death. Chronic constipation, respiratory depression, and organ failure compound the misery.

Ketamine’s Devastating Harms, Especially on Young People
- Ketamine is often sold as a grainy white or light brown powder. Looks similar to cocaine but is a very different drug. Ketamine is a general anaesthetic so it reduces sensations in the body. Trips can last for a couple of hours. Also called: K, Ket, Special K, Super K, or Vitamin K. If you take too much ketamine you may lose the ability to move and go into a ‘k-hole’. This feels like your mind and body have separated and you can’t to do anything about it. Ketamine isn’t even central to the Green Party’s list, but it’s a perfect example of why legalising hard drugs would amplify existing crises. It is already wreaking havoc on young people’s bladders, kidneys, stomachs, and mental health across the UK and beyond, and making it legally available would only make it more accessible and normalised.
- Bladder and Urinary Tract Damage: Chronic ketamine abuse causes “ketamine cystitis” or “ketamine bladder syndrome,” leading to inflammation, scarring, ulcers, and a shrunken bladder. Users experience excruciating pain, frequent urination (up to 60+ times a day), blood in urine, incontinence, and urgency. In severe cases, the bladder must be surgically removed, and damage extends to the ureters and kidneys, causing hydronephrosis (swelling), reflux, obstruction, papillary necrosis, and potential renal failure requiring dialysis. Up to 30% of heavy users develop this, and it’s increasingly hitting young people aged 16-24, with UK urology departments reporting surges in admissions for bladder inflammation. Even recreational use can lead to irreversible damage, and symptoms like frequency and cystitis-like pain can escalate to life-altering conditions.
- Kidney and Stomach Issues: Secondary renal damage from bladder dysfunction often leads to kidney scarring, infections, and failure. Stomach problems include “K-cramps”, severe abdominal pain from bile duct damage, which can require emergency care and lead to liver inflammation, chronic ulcers, or failure needing transplantation. Cholestasis (blocked bile flow) is another risk.
- Mental Health and Cognitive Damage: Long-term use triggers depression, anxiety, psychosis, hallucinations, paranoia, cognitive impairment (memory loss, reduced attention, problem-solving issues), and mood disorders. It can worsen pre-existing conditions and cause “K-hole” dissociation. A 2025 BBC report notes rising dependence, trauma, and self-harm among young users.
- These harms are already epidemic among youth, with cheap, “safe” perceptions fuelling use (8.5% of 16-59-year-olds in England/Wales tried illicit drugs in 2016/17, ketamine popular). This rising dependence amongst teenagers and young adults has and can lead to self-harm, family strain and breakdowns negative educational impacts and reduced job prospects.

The Dangers of GHB: From Coma Risks to Cognitive Impairment
- GHB, also called: 1, 4-Bd, Gbh, Gbl, Geebs, Liquid Ecstasy and often called the “date-rape drug,” depresses the central nervous system, causing euphoria but risking overdose with just a small excess. GHB and GBL can reduce people’s inhibitions, and some people take the drugs to have more intense sex. Long-term use leads to dependence, with withdrawal symptoms like anxiety, tremors, hallucinations, and high blood pressure; potentially life-threatening. Chronic abuse causes memory problems, heart disease, extreme anxiety, breathing issues, and psychiatric disorders like depression and psychosis.
- In young users, repeated comas can be neurotoxic, impairing cognition, long-term memory, and working memory, while raising stress and anxiety levels. Sexual dysfunction, liver/kidney damage, and amnesia are common.
- GHB has almost no smell and a salty/soapy taste. GBL has a very strong chemical taste and smell. Club availability could spike misuse, especially for assaults, contradicting claims of “safe” limited use. The Sexual Offences Act 2003 states that it is an offence to administer a substance, like GHB and GBL, to a person with intent to overpower that person to enable sexual activity with them. This is punishable by up to 10 years imprisonment.

The Risks of Cannabis: Mental Health Decline, Cognitive Impairment, and Dependency
The mental health and cognitive impacts of cannabis are among its most concerning long-term effects, with evidence linking regular use to permanent or semi-permanent changes in brain function. Heavy consumption, especially starting in adolescence when the brain is still developing, can impair concentration, memory, and executive functioning, leading to difficulties in learning, problem-solving, and daily performance. Structural brain changes have been observed, such as alterations in white matter integrity and accelerated aging-like effects in certain regions. Mental illness risks rise markedly: cannabis use is associated with increased likelihood of anxiety, depression, paranoia, and, crucially, psychotic disorders including full-blown psychosis and schizophrenia, particularly in those with genetic predispositions, early onset of use, or high-THC products. These effects can manifest as hallucinations, delusions, disorganised thinking, or persistent paranoia, sometimes triggering or worsening existing conditions and requiring medical intervention.

Cannabis, classified as a Class B drug in the UK, remains one of the most widely used illicit substances despite substantial evidence of its long-term harms. Cannabis is a plant-based drug. It can be smoked, eaten or vaped, it has various names including; Bhang, Bud, Dope, Draw, Ganja, Grass, Hash, Hashish, Herb, Marijuana, Pollen, Pot, Puff, Resin, Sensi, Sinsemilla, Skunk, Weed, MJ and many more. While often viewed as relatively benign compared to harder drugs, chronic or heavy use; particularly of high-potency varieties, can lead to significant physical destruction.
Smoking cannabis irritates the respiratory system, contributing to persistent cough, bronchitis, and other lung problems similar to those seen in tobacco users. A particularly distressing condition associated with long-term, frequent use is cannabinoid hyperemesis syndrome (CHS), which causes cycles of severe nausea, uncontrollable vomiting, and intense abdominal pain; sufferers often find temporary relief only through hot showers or baths, but the condition can lead to dehydration, emergency hospital visits, and complications like acute kidney injury if untreated. Additionally, cardiovascular risks emerge with prolonged exposure, including elevated heart rate and potential strain on the heart, exacerbating issues in vulnerable individuals.
- Addiction and broader societal consequences further compound these risks, as tolerance develops quickly with regular use, prompting users to consume larger amounts for the same effect and fostering dependency in a notable subset of users. Withdrawal symptoms include; irritability, insomnia, vivid dreams, low mood, poor concentration, paranoia and intense cravings, which can make quitting challenging and contribute to relapse. Youth face heightened vulnerability, with early or frequent use linked to greater risks of mental health disorders, learning difficulties, behavioural problems, and disrupted educational or social development, potentially setting the stage for lifelong challenges.
- Evidence from jurisdictions like Canada, where recreational cannabis was legalised in 2018, indicates that legalisation often correlates with increased use prevalence, including modest rises in adult consumption frequency, daily or near-daily patterns among certain groups, and shifts toward higher-potency products or edibles, though adolescent use has shown more mixed or stable trends in some studies. These patterns underscore concerns that greater availability and normalisation can amplify public health burdens without adequate safeguards.
Other Drugs; A Briefer Overview:
Methamphetamine: Brain and Body Decay: Part of the amphetamine family of stimulant drugs. Also called: Crank, Crystal, Meth, Glass, Ice, Meth, Tina And Christine, and Yaba. Methamphetamine can reduce your appetite and make you feel: exhilarated, alert, awake, agitated, paranoid, confused, aggressive and aroused:
- Medical Harms: Physical; “meth mouth,” skin sores, heart disease, strokes, and immune suppression. Mental; dopamine depletion, anhedonia (reduced ability or inability to experience pleasure and motivation, often manifesting as a core symptom of depression, schizophrenia, and other mental health disorders), psychosis, and cognitive impairments.
- Social Harms: Violence/paranoia fuels crime; dependency causes job loss, homelessness.
LSD: Persistent Psychological Trauma: LSD is a chemical usually sold in tiny amounts on blotter paper, as a liquid, or a pellet/micro-dot. It can also be called: Acid, Blotter, Dots, Drop, Liquid Acid, Lucy, Micro Dot, Tab, Tripper, Trips, and Window. For most people, the world appears distorted when they take LSD. Colours, sounds, objects and even time can all seem very strange and disturbing. LSD feeds off your imagination so every person’s experience is unique. How the trip goes will be affected by how much you take, your surroundings, who you’re with and how comfortable you are with them, as well as by your mood.

Medical Harms: Physical harms; are limited, there’s no evidence to suggest that LSD does any long-term physical damage. However, people have been known to harm themselves during a bad trip. So people in a bad mood, feeling depressed or worried should avoid taking the drug. Some people experience HPPD (Hallucinogen Persisting Perception Disorder). Mental; If you have mental health problems, or a history of mental health problems in your family, taking LSD could make them worse. Other mental health issues include: flashbacks, anxiety, depression, psychosis, schizophrenia trigger, memory/attention deficits, suicide risk.
Social Harms: Psychological dependence disrupts relationships, work; youth vulnerability to latent mental issues, especially if there is a genetic predisposition.

MDMA (Ecstasy): Serotonin Depletion and Long-Term Brain Changes: Ecstasy is primarily a recreational/club drug taken as ecstasy pills or as MDMA powder. It has several names, some are: Crystal, Dizzle, E, MD, MDMA, Mandy, Molly, Pills, Xtc. Most people feel: very happy; hence the name or ‘loved up’ feeling love and affection for the people they’re with and the strangers around them, also energised and alert. It can make people feel more in tune with their surroundings and like the music is more intense, which is why people sometimes take it in nightclubs and at parties. Some users have reported feelings of: anxiety, panic attacks, confused episodes, paranoia and even psychosis after taking ecstasy
- Medical Harms: Physical; the strength of ecstasy pills are so unpredictable and can cause overheating, dehydration, heart strain, liver damage, impotence, and weight loss. Mental; anxiety, depression, verbal memory deficits, hippocampal shrinkage (10.5% smaller), Alzheimer’s risk. Anyone with a heart condition, blood pressure problems, epilepsy or asthma can have a very dangerous reaction to the drug. While MDMA is often perceived as relatively safe among recreational users, it has been linked to serious acute harms in the UK, including fatalities and severe medical complications. Official data from the Office for National Statistics show that MDMA/ecstasy-related deaths in England and Wales have fluctuated but trended upward in recent years, with figures such as 79 deaths recorded in 2023 where MDMA or ecstasy was mentioned on the death certificate, and numbers reaching higher levels in some prior years (e.g., peaks around 80–90 in certain periods since 2018). These deaths often involve factors like hyperthermia (dangerously high body temperature), multi-organ failure, serotonin syndrome, contaminated or high-purity batches, polydrug use, or water intoxication leading to hyponatremia (low blood sodium).
- Social Harms: Tolerance leads to risky behaviour, crime; it disrupts social functioning.

Amphetamines: Stimulation Leading to Exhaustion: Amphetamine is a powerful stimulant that keeps people alert, usually sold as an off-white or pinkish powder, that sometimes look like small crystals. It is also known as: Amphetamine Sulphate, Base, Billy, Paste, Speed, Sulph, and Whizz. Some people take it because it gives them the energy to do things for hours without getting tired, like dancing. It stops you feeling hungry too, and amphetamines were once the main ingredient in diet pills. Users can also feel agitated or panicked.
- Medical Harms: Physical; heart failure, high BP, stroke, immune suppression, “meth mouth,” neurological damage. Depending on how much is taken, it can be difficult to relax or sleep, leading to insomnia. Viral hepatitis and HIV can be spread by users sharing needles, syringes or other injecting equipment. Mental; psychosis, aggression, depression, paranoia, cognitive deficits. Some people have become psychotic and delusional when on speed, which means seeing or hearing things that aren’t there.
- Social Harms: Psychological dependency causes withdrawal fatigue, job/relationship loss; youth growth stunting, crime increase.
Psilocybin (Magic Mushrooms): Hallucinogenic Risks: Magic mushrooms, ‘Shrooms or ‘magic mushrooms’ grow in the wild. They can be swallowed or made into tea. Other names for them are: Agaric, Amani, Liberties, Liberty Caps, Magics, Mushies and Philosopher’s Stones. For most people, the world appears distorted when they take mushrooms. Colours, sounds, objects and even time can all seem very different. Some people get mild hallucinations, which are also called ‘visuals’.
- Medical Harms: The biggest danger to your health when taking magic mushrooms is eating a poisonous mushroom by mistake. Physical; nausea, diarrhoea, accidents, as you can lose complete control of what you’re doing, and put yourself at risk. Mental; If you have any mental health issues, magic mushrooms can make them worse. they can also cause flashbacks, HPPD, anxiety, paranoia, trauma, depersonalisation, psychosis, insomnia, re-traumatisation in PTSD.
- Social Harms: Psychological risks disrupt daily life, relationships; emergencies from bad trips.

- Arguments against legalisation and decriminalisation include concerns over any potential increase in substance use disorders. However, psychedelics are currently being studied as a potential treatment for substance use disorders and are not considered addicting themselves. Other concerns include potential increases in psychedelic-related emergencies, such as emergency department visits for “bad trips.” Blest-Hopely: “Psychedelics are extremely powerful substances,” she says. “Any change in legislation towards better access, I would welcome greatly. However, it must come with education around psychedelics in their totality. Not just the positives, but also the risks, the effects and the enormity of impact that using large doses of substance can have, acutely and long term.”
Benzodiazepines: Sedative Dependency: Benzodiazepines are prescription drugs that can be used to treat anxiety. ‘Street benzos’ are illicit drugs that are similar but can be far more dangerous. Some drugs are increasingly cut with dangerous synthetic opioids like nitazenes, which have killed 100s of people in the UK in the past year. Other names include: Alprazolam, Bars, Benzos, Blues, Diazepam, Downers, Etizolam, Rohypnol, Roofies, Temazepam, Valium, Vallies, Xanax, and Xans. They depress the nervous system and slow the brain and body down. Benzodiazepines are often used as chill-out drugs after parties, to help people sleep after taking stimulants. Some people use them to help come down off acid, cocaine, speed or ecstasy after a big night out.
Arguments against legalisation and decriminalisation include concerns over any potential increase in substance use disorders. However, psychedelics are currently being studied as a potential treatment for substance use disorders and are not considered addicting themselves. Other concerns include potential increases in psychedelic-related emergencies, such as emergency department visits for “bad trips.” Blest-Hopely: “Psychedelics are extremely powerful substances,” she says. “Any change in legislation towards better access, I would welcome greatly. However, it must come with education around psychedelics in their totality. Not just the positives, but also the risks, the effects and the enormity of impact that using large doses of substance can have, acutely and long term.”
Benzodiazepines: Sedative Dependency: Benzodiazepines are prescription drugs that can be used to treat anxiety. ‘Street benzos’ are illicit drugs that are similar but can be far more dangerous. Some drugs are increasingly cut with dangerous synthetic opioids like nitazenes, which have killed 100s of people in the UK in the past year. Other names include: Alprazolam, Bars, Benzos, Blues, Diazepam, Downers, Etizolam, Rohypnol, Roofies, Temazepam, Valium, Vallies, Xanax, and Xans. They depress the nervous system and slow the brain and body down. Benzodiazepines are often used as chill-out drugs after parties, to help people sleep after taking stimulants. Some people use them to help come down off acid, cocaine, speed or ecstasy after a big night out.
Arguments against legalisation and decriminalisation include concerns over any potential increase in substance use disorders. However, psychedelics are currently being studied as a potential treatment for substance use disorders and are not considered addicting themselves. Other concerns include potential increases in psychedelic-related emergencies, such as emergency department visits for “bad trips.” Blest-Hopely: “Psychedelics are extremely powerful substances,” she says. “Any change in legislation towards better access, I would welcome greatly. However, it must come with education around psychedelics in their totality. Not just the positives, but also the risks, the effects and the enormity of impact that using large doses of substance can have, acutely and long term.”
Benzodiazepines: Sedative Dependency: Benzodiazepines are prescription drugs that can be used to treat anxiety. ‘Street benzos’ are illicit drugs that are similar but can be far more dangerous. Some drugs are increasingly cut with dangerous synthetic opioids like nitazenes, which have killed 100s of people in the UK in the past year. Other names include: Alprazolam, Bars, Benzos, Blues, Diazepam, Downers, Etizolam, Rohypnol, Roofies, Temazepam, Valium, Vallies, Xanax, and Xans. They depress the nervous system and slow the brain and body down. Benzodiazepines are often used as chill-out drugs after parties, to help people sleep after taking stimulants. Some people use them to help come down off acid, cocaine, speed or ecstasy after a big night out.
- Medical Harms: Physical; It is dangerous to take benzodiazepines with alcohol and/or other drugs. Alcohol and some drugs depress the central nervous system, which affects your breathing. The drugs that do this include benzodiazepines, heroin and other opioids, pregabalin and gabapentin. This means that using any combination of these types of drugs with or without alcohol increases the risk of overdose and death. People who use a lot of benzodiazepines can experience bad withdrawal symptoms, which can include tremors, nausea, vomiting, headaches, anxiety, panic attacks and depression. People going through these withdrawal symptoms might experience fits. There are concerns that benzodiazepines have been used in sex crimes, where a victim’s drink is spiked with a benzodiazepine, for example flunitrazepam (Rohypnol), making them very drowsy or knocking them out so they’re either unaware of, or unable to, prevent a sexual assault. Mental; Benzodiazepine use can negatively affect your mental health and may increase the risk of suicidal thoughts particularly in young adults and those who are alcohol or opioid dependent. they have also caused memory issues, confusion, depression, anxiety, cognitive impairment.
- Social Harms: High dependency/withdrawal (seizures), often laced with synthetics; crime for acquisition, loss of job/home/family.
Anabolic Steroids: Body Image-Driven Damage: Anabolic steroids are generally taken as tablets or injected liquid, that some people take to build muscles or improve sports performance, they allow them to be able to train harder and longer and help them to recover from strenuous exercise faster. Other names are: Juice, Melanotan, Nootropics, Roids, Sildenafil, Smart drugs and Viagra

- Medical Harms: Taking anabolic steroids does involve risks to your body and health. Physical; If you’re male, regular use can lead to erection problems, growing of breasts, becoming sterile, loss of hair and development of acne. It can also make your testicles shrink. If you’re female, you can develop more masculine characteristics – with extra facial hair, loss of hair on the head, a deeper voice, shrinking breasts, and an enlarged clitoris; as well as risking acne, an increased risk of menstrual problems and changes in sex drive. Steroids can also give you high blood pressure and increase your risk of illness and death due to liver failure, stroke or heart attack. If you’re young, anabolic steroids can mess up how your body develops, stopping you from growing properly. Injecting any drug, even steroids, can damage your veins and cause ulcers and gangrene, particularly with dirty needles or poor injecting technique. Sharing needles, syringes and other injecting works can help spread HIV, hepatitis C and other infections. Mental; Because anabolic steroids can make you feel paranoid, aggressive and violent for no reason, it’s not that unusual for anabolic steroid users to lash out or attack family and friends, known as “roid rage,” paranoia, mood swings and trouble sleeping.
- Social Harms: Dependency, injection risks (infections); Criminal convictions related to violence, Family breakdowns, youth misuse for aesthetics.
Potential Devastating Impacts on UK Society and the NHS
Legalising hard drugs would place severe additional strain on the UK, a country already grappling with rising drug-related deaths. In England and Wales, there were 5,448 deaths related to drug poisoning registered in 2023; the highest number since records began in 1993, representing an 11% increase from 4,907 in 2022 (source: Office for National Statistics via various reports, including ONS bulletins and media coverage). Societal harms would likely intensify under such a policy. Increased addiction, crime, and violence could become more prevalent, with the potential for a surge in youth use, as observed in places like the Netherlands and Canada following reforms to cannabis policies (various studies and BBC reporting). Family breakdowns, homelessness, and exploitation might rise further, exacerbating existing social issues. The economic costs of drug misuse, already estimated at around £20 billion per year for society (including crime and health impacts), could balloon significantly (National Audit Office report, 2023). The NHS would face particularly heavy burdens. Expert opinions have warned of billions in extra costs arising from surges in demand for addiction treatment, emergency care, and mental health services related to crises. An already stretched NHS could become overwhelmed, similar to patterns seen in Canada and the US, where hospitalisations linked to drug use have increased following certain liberalisation measures. Overall, these factors highlight the potential for devastating, multifaceted impacts on UK society and public health services if hard drugs were legalised.

Counterarguments and Refutations: Addressing Pro-Legalisation Views
Pro-legalisation advocates, including organisations like Transform Drug Policy Foundation, argue for reforms such as legalising and regulating certain drugs (e.g., cannabis) to control markets, reduce harms, and generate benefits. Here, the strongest points from diverse sources are presented and refuted based on available evidence.
- Refutation: Personal freedom does not justify the broader societal costs, including irreversible damage and deaths. Stigma can persist even after policy changes (e.g., in British Columbia post-decriminalisation efforts), and evidence suggests that overall harms outweigh arguments for liberty in many cases.
- Argument: Legalisation reduces crime and dismantles black markets: Proponents claim that legalisation would eliminate illegal markets, thereby reducing associated violence and freeing up policing resources.
- Refutation: Evidence indicates that black markets often persist alongside legal ones, and violence can shift rather than disappear (e.g., turf wars in legal cannabis states). In places like Oregon (following Measure 110 decriminalisation) and Portugal, crime trends have varied, with some recent increases noted before policy reversals in Oregon; proposed UK policing savings (around £1.4 billion) may be outweighed by new societal harms from increased use.
- Argument: Generates tax revenue and economic benefits: Legalisation could produce billions in tax revenue to fund public services.
- Refutation: Net costs frequently exceed revenues, as health and societal burdens rise with greater drug use. The UK’s current economic costs of drug misuse are estimated at around £20 billion per year (including crime and health impacts), and these could increase further, as seen in Canada and the US where hospitalisations and other harms have offset fiscal gains.
- Argument: Improves public health through regulation and harm reduction: Regulated markets would provide safer products and better access to treatment.
- Refutation: Drug use often increases post-liberalisation (e.g., in Canada following cannabis legalisation and in Portugal over longer terms despite initial decriminalisation successes), leading to more harms overall. Regulation does not fully prevent addiction or overdoses, with spikes observed in issues like cannabis-related hospitalisations in Canada.
- Argument: Enhances personal freedom and reduces stigma: Adults should have the choice to use drugs, and criminalisation causes more harm than the substances themselves.
These refutations underscore fundamental value conflicts: while pro-legalisation views prioritise liberty and potential economic gains, substantial evidence points to net increases in harms.
Evaluation: Synthesising Evidence for a Balanced Assessment
Synthesising findings from medical and policy sources (e.g., NIDA, CAMH, Priory Group), hard drugs cause irreversible harms including addiction, mental health crises, and fatalities. Global experiences with liberalisation often show increased use and harms without delivering promised benefits. In the UK context, risks include overwhelming the already strained NHS with billions in extra costs for treatment, emergencies, and related care, alongside broader societal disruption. While some decriminalisation models (e.g., Portugal’s early approach) reduced deaths through a strong focus on treatment and health services, full legalisation tends to amplify risks without equivalent gains. Pro-legalisation arguments often overlook these value conflicts and the weight of evidence indicating net societal harm from expanded access to hard drugs.
Conclusion: Reject Radical Legalisation for Evidence-Based Alternatives
The Green Party’s proposals to legalise all drugs, including crack cocaine, heroin, and substances like GHB, represent a stupid, reckless gamble that could unleash widespread societal devastation across the UK, and this is just ONE of their insane policies! Unearthed policy documents suggest the party views controlled recreational drug use as potentially beneficial for “human relationships” and advocates partnerships with South American cartels for a “sustainable supply” of coca and cocaine, while pushing for cocaine drinks on high streets and Class A drugs at nightclubs and festivals.
With the UK already enduring record-high drug poisoning fatalities; 5,565 in England and Wales in 2024, marking a 12th consecutive year of increases, these radical ideas risk amplifying addiction, health crises, crime, and societal break-down, placing an intolerable burden on an already strained NHS and the broader economy.
Global evidence underscores the perils of decriminalisation and legalisation, demanding utmost caution rather than experimentation. British Columbia’s 2023 decriminalisation pilot triggered explosions in open drug consumption, discarded syringes in playgrounds, and even fentanyl smoking in hospitals, correlating with a 23% spike in opioid hospitalisations and no reduction in poisoning rates or deaths in the first 11 months. Canada’s broader cannabis legalisation, while reducing arrests, has driven up emergency department visits and hospitalisations, particularly among youth, highlighting how liberalisation boosts use and harms without delivering promised benefits.
These failures illustrate that decriminalisation and legalisation do not dismantle black markets as claimed; instead, they shift violence, persist illicit trade, and overwhelm public health systems, with net costs far exceeding any tax revenues. The UK’s escalating drug crisis further amplifies these warnings, with synthetic opioids like nitazenes linked to hundreds of excess deaths. London saw a 32% surge in drug poisonings in 2024, while national hospital stays for drug-related issues climbed to 11,136 in 2023/24, with opioids driving the highest rates at 91 per 100,000 population. This burden already costs the NHS billions annually in addiction treatment, emergencies, and mental health crises, with unnecessary prescribing of dependency-forming medicines alone draining £493-£564 million yearly. Legalisation would exacerbate this, ballooning economic losses from £20 billion per year in societal costs; including crime, family breakdowns, and homelessness, while straining resources amid rising cocaine-related deaths and opioid poisonings.

Prioritising personal freedom ignores these irreversible harms, as stigma and societal fallout persist post-reform, outweighing any liberty gains. Instead, evidence demands rejecting radical legalisation in favour of compassionate, proven alternatives that reduce harms without encouraging use. The UK’s 10-year drugs plan emphasises robust treatment expansion, like opioid agonist therapy, which cuts mortality, overdose, and infections harm reduction measures such as needle programmes and naloxone distribution, and targeted enforcement on supply chains to disrupt criminal networks. These interventions, backed by cross-government innovation funds, have demonstrated cost-effectiveness, improving recovery rates and saving lives without the spikes in use seen in liberalised regimes. Portugal’s early successes stemmed not from decriminalisation alone but from heavy investment in health services, a lesson the UK should heed by bolstering existing strategies rather than overhauling them.
Radical proposals like the Green Party’s are dangerously out of touch with this evidence, prioritising ideology over public safety; true reform lies in evidence-based, health-focused policies that address root causes like deprivation and adverse experiences, ensuring a safer society for all.
References and Additional Resources:
- Ali, F. et al. (2025) ‘Experiences of stigmatization among people who use drugs in the initial year of British Columbia’s drug decriminalization policy: A qualitative study’, International Journal of Drug Policy, 128, p. 104458. doi: 10.1016/j.drugpo.2025.104458.
- American Addiction Centers (2024) Long-Term Side Effects of Cocaine on the Brain & Body. Available at: https://americanaddictioncenters.org/stimulants/cocaine/long-term-side-effects-of-abuse (Accessed: 21 February 2026).
- Askew, R. et al. (2025) ‘Why are people with lived and living experience conflicted about the legalisation of drugs? A thematic analysis’, International Journal of Drug Policy, 128, p. 104458. doi: 10.1016/j.drugpo.2025.104458.
- Barata, P.C. et al. (2021) ‘Non-medical cannabis use: international policies and outcomes overview. An outline for Portugal’, Drug and Alcohol Dependence, 228, p. 109006. doi: 10.1016/j.drugalcdep.2021.109006.
- Better Health Channel (n.d.) Amphetamines. Available at: https://www.betterhealth.vic.gov.au/health/healthyliving/amphetamines (Accessed: 21 February 2026).
- Better Health Channel (n.d.) Heroin. Available at: https://www.betterhealth.vic.gov.au/health/healthyliving/heroin (Accessed: 21 February 2026).
- Better Health Channel (n.d.) MDMA (ecstasy). Available at: https://www.betterhealth.vic.gov.au/health/healthyliving/mdma-ecstasy (Accessed: 21 February 2026).
- Bonnet, U. et al. (2020) ‘Ranking the Harm of Psychoactive Drugs Including Prescription Analgesics to Users and Others–A Perspective of German Addiction Medicine Experts’, Frontiers in Psychiatry, 11, p. 592199. doi: 10.3389/fpsyt.2020.592199.
- CAMH (n.d.) GHB. Available at: https://www.camh.ca/en/health-info/mental-illness-and-addiction-index/ghb (Accessed: 21 February 2026).
- CAMH (n.d.) LSD. Available at: https://www.camh.ca/en/health-info/mental-illness-and-addiction-index/lsd (Accessed: 21 February 2026).
- Carhart-Harris, R.L. et al. (2016) ‘The paradoxical psychological effects of lysergic acid diethylamide (LSD)’, Psychological Medicine, 46(7), pp. 1379-1390. doi: 10.1017/S0033291715002901.
- Cheng, G.L.F. et al. (2013) ‘Heroin abuse accelerates biological aging: a novel insight from telomerase and brain imaging interaction’, Translational Psychiatry, 3, p. e260. doi: 10.1038/tp.2013.36.
- Cleveland Clinic (2023) Cocaine (Crack): What It Is, Side Effects, Risks & Withdrawal. Available at: https://my.clevelandclinic.org/health/articles/4038-cocaine-crack (Accessed: 21 February 2026).
- Cregler, L.L. and Mark, H. (1989) ‘Adverse health consequences of cocaine abuse’, Journal of the National Medical Association, 81(1), pp. 27-38.
- Dalgarno, P. (2021) ‘Illegal drugs in the UK: Is it time for considered legalisation to improve public health?’, Drug Science, Policy and Law, 7, p. 1-10. doi: 10.1177/20503245211005348. https://www.drugsandalcohol.ie/34187/ https://www.researchgate.net/publication/351164369_Illegal_drugs_in_the_UK_Is_it_time_for_considered_legalisation_to_improve_public_health (Accessed: 21 February 2026).
- Dills, A. et al. (2021) The Effect of State Marijuana Legalizations: 2021 Update. Cato Institute. Available at: https://www.cato.org/policy-analysis/effect-state-marijuana-legalizations-2021-update (Accessed: 21 February 2026).
- Drug Free CT (n.d.) Long-Term Effects of Methamphetamine Use. Available at: https://www.drugfreect.org/substance-info/other-drugs/methamphetamine/long-term-effects (Accessed: 21 February 2026).
- European College of Neuropsychopharmacology (2018) Club drug GHB associated with brain and cognitive changes. Available at: https://www.sciencedaily.com/releases/2018/10/181008104628.htm (Accessed: 21 February 2026).
- Faiola, A. and Martins, C.F. (2023) ‘Once hailed for decriminalizing drugs, Portugal is now having doubts’, The Washington Post, 7 July. Available at: https://www.washingtonpost.com/world/2023/07/07/portugal-drugs-decriminalization-heroin-crack (Accessed: 21 February 2026).
- Fernandes, C. (2025) Examining Drug Policy in Portugal and Greece. CUNY Academic Works. Available at: https://academicworks.cuny.edu/cgi/viewcontent.cgi?article=2312&context=cc_etds_theses (Accessed: 21 February 2026).
- Gonçalves, R. et al. (2025) ‘Measuring drug policy evolution: a new era for harm reduction’, International Journal of Drug Policy, 128, p. 104458. doi: 10.1016/j.drugpo.2025.104458.
- Greenhouse Treatment Center (2024) Health Risks & Effects of Heroin Use. Available at: https://greenhousetreatment.com/heroin-treatment/effects (Accessed: 21 February 2026).
- Hall, A.P. and Henry, J.A. (2006) ‘Acute toxic effects of ‘Ecstasy’ (MDMA) and related compounds: overview of pathophysiology and clinical management’, British Journal of Anaesthesia, 96(6), pp. 678-685. doi: 10.1093/bja/ael078.
- Healthdirect (2025) GHB: Party Drug and Date Rape Drug. Available at: https://www.healthdirect.gov.au/ghb (Accessed: 21 February 2026).
- Healthdirect (2025) LSD (acid). Available at: https://www.healthdirect.gov.au/lsd-acid (Accessed: 21 February 2026).
- Healthdirect (2025) MDMA (ecstasy). Available at: https://www.healthdirect.gov.au/mdma-ecstasy (Accessed: 21 February 2026).
- Holland, A. (2020) ‘An ethical analysis of UK drug policy as an example of a criminal justice approach to drugs’, BMC Medical Ethics, 21, p. 42. doi: 10.1186/s12910-020-00485-4.
- Imperial College London (2013) Long-term cannabis use may blunt the brain’s motivation system. Available at: https://www.imperial.ac.uk/news/124806/long-term-cannabis-blunt-brains-motivation-system (Accessed: 21 February 2026).
- Imperial College London (2022) Magic mushroom compound increases brain connectivity in people with depression. Available at: https://www.imperial.ac.uk/news/235514/magic-mushroom-compound-increases-brain-connectivity (Accessed: 21 February 2026).
- King’s College London (2025) Largest ever study into cannabis use investigates risk of paranoia and poor mental health in the general population. Available at: https://www.kcl.ac.uk/news/largest-ever-study-into-cannabis-use-investigates-risk-of-paranoia-and-poor-mental-health-in-the-general-population (Accessed: 21 February 2026).
- King’s College London (2025) Psychedelic Trials Group. Available at: https://www.kcl.ac.uk/research/psychoactive-trials-group (Accessed: 21 February 2026).
- Kopra, E.I. et al. (2022) ‘Adverse experiences resulting in emergency medical treatment seeking following the use of magic mushrooms’, Journal of Psychopharmacology, 36(8), pp. 965-973. doi: 10.1177/02698811221084063.
- Liberty House Clinic (2024) Amphetamine Addiction | Signs, Symptoms and Effects. Available at: https://www.libertyhouseclinic.co.uk/drug-addiction/amphetamine (Accessed: 21 February 2026).
- Manchester University NHS Foundation Trust (2021) Cannabis and mental health. Available at: https://mft.nhs.uk/app/uploads/2021/01/Cannabis-and-mental-health.pdf (Accessed: 21 February 2026).
- McKetin, R. et al. (2019) ‘Mental health outcomes associated with the use of amphetamines: A systematic review and meta-analysis’, EClinicalMedicine, 16, pp. 81-97. doi: 10.1016/j.eclinm.2019.09.014.
- MedlinePlus (2024) Substance use – amphetamines. Available at: https://medlineplus.gov/ency/patientinstructions/000792.htm (Accessed: 21 February 2026).
- Mental Health Foundation (2021) Drugs and mental health. Available at: https://www.mentalhealth.org.uk/explore-mental-health/a-z-topics/drugs-and-mental-health (Accessed: 21 February 2026).
- Merriman, S. (2026) ‘Outcry as Green Party say they want to legalise ALL drugs – including crack cocaine, heroin and date-rape chemical GHB’, Daily Mail, 20 February. Available at: https://www.dailymail.co.uk/news/article-15579401/Green-Party-legalise-drugs-crack-cocaine-heroin-date-rape-chemical-GHB.html?ns_mchannel=rss&ns_campaign=1490&ito=social-twitter_mailonline (Accessed: 21 February 2026).
- Millsaps, F. (2023) Decriminalizing Drugs: A Comparative Study of Oregon in an International Context. PDXScholar. Available at: https://pdxscholar.library.pdx.edu/cgi/viewcontent.cgi?article=2664&context=honorstheses (Accessed: 21 February 2026).
- Mind (n.d.) How drugs and alcohol can affect your mental health. Available at: https://www.mind.org.uk/information-support/types-of-mental-health-problems/recreational-drugs-alcohol-and-addiction/how-drugs-and-alcohol-can-affect-your-mental-health (Accessed: 21 February 2026).
- Mohebbian, M. et al. (2025) ‘Exploring the impact of drug decriminalization and legalization policies on mental health outcomes: A scoping review’, PLOS Mental Health, 2(9), p. e0000358. doi: 10.1371/journal.pmen.0000358.
- Morgan, N. et al. (2025) ‘Drug decriminalization: a co-designed study outlining the implications for providers of youth services’, PMC, PMC12539142.
- Moury, C. et al. (2023) ‘Understanding successful policy innovation: The case of Portuguese drug policy’, Addiction, 118(6), p. 1153-1163. doi: 10.1111/add.16099.
- National Institute on Drug Abuse (n.d.) What are the long-term effects of heroin use?. Available at: https://nida.nih.gov/publications/research-reports/heroin/what-are-long-term-effects-heroin-use (Accessed: 21 February 2026).
- National Institute on Drug Abuse (n.d.) Methamphetamine. Available at: https://nida.nih.gov/publications/research-reports/methamphetamine/what-are-long-term-effects-methamphetamine-misuse (Accessed: 21 February 2026).
- National Toxicology Program (2005) NTP-CERHR monograph on the potential human reproductive and developmental effects of amphetamines. Available at: https://ntp.niehs.nih.gov/ntp/ohat/stimulants/amphetamines/amphetaminesmonofinal_508.pdf (Accessed: 21 February 2026).
- NHS (n.d.) Cocaine addiction: get help. Available at: https://www.nhs.uk/live-well/addiction-support/cocaine-get-help (Accessed: 21 February 2026).
- NHS (n.d.) Medical cannabis (cannabis oil). Available at: https://www.nhs.uk/medicines/medical-cannabis (Accessed: 21 February 2026).
- NHS (n.d.) Overview – Psychosis. Available at: https://www.nhs.uk/mental-health/conditions/psychosis/overview (Accessed: 21 February 2026).
- NHS Inform (2022) Cannabis. Available at: https://www.nhsinform.scot/healthy-living/drugs-and-drug-use/common-drugs/cannabis (Accessed: 21 February 2026).
- NHS Inform (2024) MDMA (Ecstasy). Available at: https://www.nhsinform.scot/healthy-living/drugs-and-drug-use/common-drugs/mdma-ecstasy (Accessed: 21 February 2026).
- NHS Inform (2025) Cocaine. Available at: https://www.nhsinform.scot/healthy-living/drugs-and-drug-use/common-drugs/cocaine (Accessed: 21 February 2026).
- NIDA (n.d.) What are the long-term effects of heroin use?. Available at: https://nida.nih.gov/publications/research-reports/heroin/what-are-long-term-effects-heroin-use (Accessed: 21 February 2026)
- Nguyen, H.V. (2025) ‘Safer Opioid Supply, Subsequent Drug Decriminalization, and Opioid Overdoses’, JAMA Health Forum, 6(3), p. e250000. doi: 10.1001/jamahealthforum.2025.0000. https://jamanetwork.com/journals/jama-health-forum/fullarticle/2831562 (Accessed: 21 February 2026)
- Oxford Health NHS Foundation Trust (2024) Study finds brain function and structure changes in lifetime cannabis users. Available at: https://oxfordhealth.nhs.uk/news/study-finds-brain-function-and-structure-changes-in-lifetime-cannabis-users (Accessed: 21 February 2026).
- Priory Group (n.d.) Amphetamine Addiction Treatment. Available at: https://www.priorygroup.com/addiction-treatment/amphetamine-addiction-treatment (Accessed: 21 February 2026).
- Priory Group (n.d.) Crack Cocaine. Available at: https://www.priorygroup.com/blog/crack-cocaine (Accessed: 21 February 2026).
- Priory Group (n.d.) Long-term effects of ketamine. Available at: https://www.priorygroup.com/blog/long-term-effects-of-ketamine (Accessed: 21 February 2026).
- Priory Group (n.d.) The short and long-term effects of cocaine on the body. Available at: https://www.priorygroup.com/blog/the-short-and-long-term-effects-of-cocaine-on-the-body (Accessed: 21 February 2026).
- Providence Project (2024) Amphetamine Abuse Statistics in the UK. Available at: https://providenceproject.org/addiction/drugs/amphetamines/stats-and-facts (Accessed: 21 February 2026).
- PTSD UK (n.d.) Psychedelic-Assisted Therapy for PTSD and C-PTSD: A Responsible Approach. Available at: https://www.ptsduk.org/psychedelic-assisted-therapy (Accessed: 21 February 2026).
- Rehabs UK (n.d.) What’s Behind The Recent Rise In Cocaine Addiction In The UK?. Available at: https://rehabsuk.com/blog/what-s-behind-the-recent-rise-in-cocaine-addiction-in-the-uk (Accessed: 21 February 2026).
- Roberts, E. (2024) ‘What impact could the legalisation of recreational cannabis have on the health of the United Kingdom? Lessons from the rest of the world’, PMC, PMC7615739. pmc.ncbi.nlm.nih.gov (Accessed: 21 February 2026).
- Royal Berkshire NHS Foundation Trust (n.d.) Cannabis use – the effects on you and your baby – a guide for parents. Available at: https://www.royalberkshire.nhs.uk/media/vhqp4dsh/cannabis-use-in-pregnancy_a-parents-guide.pdf (Accessed: 21 February 2026).
- Royal College of Psychiatrists (n.d.) Cocaine dependence. Available at: https://www.rcpsych.ac.uk/mental-health/mental-illnesses-and-mental-health-problems/cocaine-dependence (Accessed: 21 February 2026).
- Rusyniak, D.E. (2013) ‘Neurologic Manifestations of Chronic Methamphetamine Abuse’, PMC, PMC3764482. https://pmc.ncbi.nlm.nih.gov/articles/PMC3764482/ (Accessed: 21 February 2026).
- SAMHSA (2024) What are Stimulants? Side Effects, Short and Long Term Risks. Available at: https://www.samhsa.gov/substance-use/learn/stimulants (Accessed: 21 February 2026).
- Scheim, A.I. et al. (2020) ‘Impact evaluations of drug decriminalisation and legal regulation on drug use, health and social harms: a systematic review’, BMJ Open, 10(9), p. e035148. doi: 10.1136/bmjopen-2019-035148.
- Schmid, Y. et al. (2017) ‘Long-lasting subjective effects of LSD in normal subjects’, Psychopharmacology, 235(2), pp. 535-545. doi: 10.1007/s00213-017-4733-3.
- South London and Maudsley NHS Foundation Trust (2025) New research on the relationship between cannabis use, risk of paranoia and poor mental health | Our blog. Available at: https://slam.nhs.uk/blog/new-research-on-the-relationship-between-cannabis-use-risk-of-paranoia-and-poor-mental-health-4678 (Accessed: 21 February 2026).
- StatCan (2023) Five years since legalization, what have we learned about cannabis in Canada?. Available at: https://www150.statcan.gc.ca/n1/daily-quotidien/231016/dq231016c-eng.htm (Accessed: 21 February 2026).
- Stevens, A. et al. (2024) ‘In defence of the decriminalisation of drug possession in the UK’, Journal of Psychedelic Studies, 8(1), p. 1-10. doi: 10.1177/20503245241239200.
- Strous, J.F.M. et al. (2022) ‘Brain Changes Associated With Long-Term Ketamine Abuse, A Systematic Review’, PMC, PMC8972190.Talk to Frank (n.d.) Anabolic steroids. Available at: https://talktofrank.com/drug/anabolic-steroids (Accessed: 21 February 2026).
- Talk to Frank (n.d.) Benzodiazepines. Available at: https://talktofrank.com/drug/benzodiazepines (Accessed: 21 February 2026).
- Talk to Frank (n.d.) Drugs A to Z. Available at: https://talktofrank.com/drugs-a-z (Accessed: 21 February 2026).
- Talk to Frank (n.d.) Honest information about drugs. Available at: https://talktofrank.com/ (Accessed: 21 February 2026).
- The Guardian (2011) Long-term ecstasy use ‘raises risk of brain damage and Alzheimer’s’. Available at: https://www.theguardian.com/society/2011/apr/06/ecstasy-brain-damage-memory-loss-alzheimers (Accessed: 21 February 2026).
- The Guardian (2024) Experts warn of mental health risks after rise in magic mushroom use. Available at: https://www.theguardian.com/science/2024/dec/25/experts-warn-of-mental-health-risks-after-rise-in-magic-mushroom-use (Accessed: 21 February 2026).
- Transform Drugs Policy Foundation (2021) Drug decriminalisation in Portugal: setting the record straight. Available at: https://transformdrugs.org/blog/drug-decriminalisation-in-portugal-setting-the-record-straight (Accessed: 21 February 2026).
- Transform Drugs Policy Foundation (n.d.) Transform Drugs. Available at: https://transformdrugs.org/ (Accessed: 21 February 2026).
- UK Anti-Doping (n.d.) What’s banned in sport – the Prohibited List. Available at: https://www.ukad.org.uk/athletes/whats-banned-sport-prohibited-list (Accessed: 21 February 2026).
- UK Government (2013) FRANK: free practical drug advice for adults and children. Available at: https://www.gov.uk/government/publications/frank (Accessed: 21 February 2026).
- UK Government (2019) Increase in crack cocaine use inquiry: summary of findings. Available at: https://www.gov.uk/government/publications/crack-cocaine-increase-inquiry-findings/increase-in-crack-cocaine-use-inquiry-summary-of-findings (Accessed: 21 February 2026).
- UK Government (2025) List of most commonly encountered drugs currently controlled under the misuse of drugs legislation. Available at: https://www.gov.uk/government/publications/controlled-drugs-list–2/list-of-most-commonly-encountered-drugs-currently-controlled-under-the-misuse-of-drugs-legislation (Accessed: 21 February 2026).
- UKAT (2025) LSD addiction | LSD abuse signs and symptoms. Available at: https://www.ukat.co.uk/addiction/drug/hallucinogens/lsd (Accessed: 21 February 2026).
- UKAT (n.d.) Long-term effects and risks of using cocaine. Available at: https://www.ukat.co.uk/blog/substance-abuse/long-term-effects-and-risks-of-using-cocaine (Accessed: 21 February 2026).
- University of Rochester Medical Center (n.d.) All About LSD. Available at: https://www.urmc.rochester.edu/encyclopedia/content?ContentID=2604&ContentTypeID=1 (Accessed: 21 February 2026).
- University Hospital Southampton (n.d.) Cannabinoid hyperemesis syndrome (CHS) – patient information. Available at: https://www.uhs.nhs.uk/Media/UHS-website-2019/Patientinformation/Emergency-medicine/Cannabinoid-hyperemesis-syndrome-CHS-2506-PIL.pdf (Accessed: 21 February 2026).
- van Amsterdam, J. et al. (2012) ‘Possible long-term effects of GHB – Neurotoxicity and overdose’, PubMed, 22342779. https://pubmed.ncbi.nlm.nih.gov/22342779/ (Accessed: 21 February 2026).
- Zoorob, M.J. et al. (2024) ‘Drug Decriminalization, Fentanyl, and Fatal Overdoses in Oregon’, JAMA Network Open, 7(9), p. e2431610. doi: 10.1001/jamanetworkopen.2024.31610. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2823254 (Accessed: 21 February 2026).
