
February 13th, 2026 – Today marks International Condom Day, an annual observance dedicated to raising awareness about the importance of condoms in preventing sexually transmitted infections (STIs), including HIV, and unintended pregnancies. Strategically placed the day before Valentine’s Day, it serves as a practical reminder that romance should always include safe practices. The campaign encourages everyone to prioritise protection, get tested, and spread the message of safer sex.
Quick Facts
- Date: Every February 13th
- Founder and Year: AIDS Healthcare Foundation (AHF), 2009
- Official Website: ahf.org/ahf-celebrates-international-condom-day and related pages like aidshealth.org
- Hashtag: #InternationalCondomDay
- Current Theme (2026): “Just Use It!” – emphasizing condoms as a powerful, cost-effective tool for HIV and STI prevention
- Global Reach: Events in nearly 50 countries, including free condom distributions, education, and creative campaigns
International Condom Day highlights condoms as an essential barrier method, promoting accessibility, stigma-free use, and empowerment in sexual health.
Chronological Timeline of Condoms and International Condom Day
The history of condoms spans millennia, evolving from rudimentary protections to modern public health essentials.
- c. 3000 BC: Earliest references to protective sheaths in ancient literature, including goat bladders (e.g., legend of King Minos), linen in Egypt, animal intestines in Rome, plant-based female sheaths in some tribes, and silk in China – primarily for disease prevention.
- c. 1564: Italian physician Gabriele Falloppio documents linen sheaths to prevent syphilis, an early European account of disease-focused use.
- 1839: Charles Goodyear patents vulcanised rubber, enabling durable, reusable rubber condoms.
- c. 1855: Rubber condoms invented and mass-produced, shifting from animal materials.
- c. 1919–1920: Latex development and dipping techniques create thinner, disposable condoms, revolutionising production.
- 1960s–1970s: Condoms integrated into global family planning as a non-hormonal contraceptive.
- Early 1980s: HIV/AIDS epidemic reframes condoms as lifesaving for reducing sexual transmission.
- 1990: WHO adds male latex condoms to its Model List of Essential Medicines.
- 1993: U.S. FDA approves internal (female) condoms, offering receptive partners control.
- 2000s: Evidence confirms consistent use reduces HIV risk by ~80% and protects against other STIs.
- 2009: AHF launches International Condom Day on February 13 to promote safer sex with the tagline “Put It On.”
- 2020s–Present: Ongoing campaigns amid rising STIs; 2026 features “Just Use It!” with global events and U.S. burlesque shows like Ohh Mamma!.
History of International Condom Day
Condom-like devices date back thousands of years for disease and pregnancy prevention. Modern latex condoms emerged in the 1920s for affordability and mass production. The 1980s HIV crisis boosted uptake worldwide. Founded by AHF in 2009 amid the AIDS response, International Condom Day uses light-hearted, creative messaging to combat stigma and encourage consistent use. Today, with HIV manageable through treatment, condoms remain vital, reducing transmission risk by about 80% when used correctly.
How to Celebrate International Condom Day
- Stock Up and Check Expiry: Ensure fresh, unexpired condoms are available.
- Visit Official Resources: Explore AHF sites for events, past photos, and education.
- Spread Awareness: Share on social media, host community events, or discuss safe sex with friends and partners.
- Get Tested: Access free HIV/STI testing via AHF or local NHS clinics.
- Learn More: Dive into HIV management and prevention through AHF resources.
Understanding STIs: Causes, Treatments, and Curability
Sexually transmitted infections (STIs), also known as STDs, are infections spread primarily through sexual contact (vaginal, anal, or oral). They are caused by more than 30 different bacteria, viruses, and parasites.
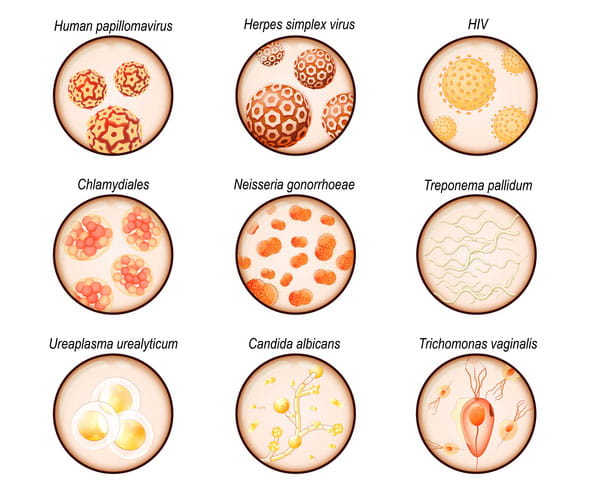
- Viral STIs (e.g., HIV, genital herpes/HSV, hepatitis B, HPV/genital warts) invade and multiply within cells; these cannot be cured but can often be managed or controlled with antiviral medications to reduce symptoms and transmission risk.
- Bacterial STIs are caused by single-celled organisms (e.g., gonorrhoea/Neisseria gonorrhoeae, syphilis/Treponema pallidum, chlamydia/Chlamydia trachomatis); they can be effectively treated and cured with antibiotics.
- Parasitic STIs involve small organisms that feed on the infected person (the “host”), such as pubic lice (crabs/Phthirus pubis), scabies (Sarcoptes scabiei mites), and trichomoniasis (Trichomonas vaginalis protozoan); these are curable with over-the-counter or prescription antiparasitic treatments.
- Curable STIs generally include chlamydia, gonorrhoea, syphilis, pubic lice, scabies, trichomoniasis, non-gonococcal urethritis (NGU, often bacterial), and related urinary tract infections (UTIs). Pelvic inflammatory disease (PID), a complication of untreated bacterial STIs like chlamydia or gonorrhoea, can be treated with antibiotics but may cause permanent scarring even after cure.
- Prevention includes consistent condom use, testing, and limiting partners. For more teen-friendly info, see KidsHealth.org on STDs. Additional resources on STIs are available at Be in the KNOW.
Key Facts
- Latex condoms are ~98% effective against pregnancy with perfect use, but ~87% with typical use due to errors.
- Consistent use reduces HIV transmission by ~80%+ and lowers risks for gonorrhoea, chlamydia, and others.
- Internal condoms offer similar pregnancy protection (~21% typical failure) with added user control.
- Condoms feature on WHO’s Essential Medicines List for preventing infections and pregnancies.
- Ancient versions were reusable linen or animal-gut sheaths focused on disease prevention.
- The AIDS epidemic drove global condom integration into HIV programs.
UK Focus: Observances, Statistics, and Initiatives
In the UK, International Condom Day aligns with efforts by organisations like Terrence Higgins Trust and NHS clinics offering free condoms, testing, and education. AHF UK supports distributions and awareness. Recent data shows challenges: STI diagnoses remain high, with over 350 daily in 15–24-year-olds in 2024, though some declines in gonorrhoea and syphilis in 2025. Condom use among adolescents has declined significantly since 2014 (e.g., from ~60% to 37–40% in Scotland/Wales for girls at last intercourse). Overall, many adults report inconsistent use, with trust in partners cited as a reason for skipping condoms. Rising STI rates underscore the need for renewed promotion.
Checklist for Correct Condom Use

Using a condom correctly maximizes protection against STIs and pregnancy. Follow this step-by-step checklist (based on UK health guidelines, e.g., NHS recommendations): https://www.malecontraceptive.org/blog/what-are-condoms
- Store condoms in a cool, dry place (avoid wallets, pockets, or hot environments that can damage them).
- Check the package for any damage or tears before opening.
- Look for the British Standard Kitemark (often heart-shaped with an “S” or similar design) and/or CE/UKCA mark, confirming the condom meets tested safety standards.
- Check the expiry date – do not use expired condoms.
- Before any genital contact, open the foil wrapper carefully (avoid teeth, nails, or jewellery that could tear it) and remove the condom.
- Ensure the penis is fully erect.
- Squeeze the teat (reservoir tip) to exclude air, then place it on the tip of the penis.
- Roll the condom down fully to the base of the penis.
- Check it’s rolled on correctly; if it’s the wrong way round, discard it and start with a new one (do not flip it, as it may have pre-ejaculate or fluids on the inside).
- Never use two condoms at once (double-bagging increases breakage risk).
- Use only water-based lubricants (e.g., KY Jelly, Pasante Lube, or Durex Play); avoid oil-based products like lotion or petroleum jelly, which degrade latex.
- After ejaculation, withdraw immediately while holding the base of the condom to prevent slippage or leakage.
- Check for any splits or tears after use.
- Wrap the used condom in tissue and dispose in a bin (not the toilet).
- Never reuse a condom – use a new one for any further sexual activity.
For visual demos and official guidance, refer to the NHS Condoms page.
How to put a condom on | NHS
FAQs
- Do condoms expire? Yes – check the date; expired ones lose effectiveness.
- Are condoms safe and effective? Properly used, ~98% effective against pregnancy; highly effective against HIV/STIs.
- Do they prevent STDs/STIs? Yes, when used correctly every time.
- Can they cause UTIs? Some lubricants/spermicides may increase risk; plain versions are generally safe.
Conclusion
International Condom Day reminds us that safe sex is essential for health, pleasure, and responsibility. Condoms remain one of the most accessible, effective tools against HIV, STIs, and unintended pregnancies. By checking supplies, getting tested, and normalising protection; especially ahead of romantic occasions, we can reduce risks and empower healthier choices. Let’s embrace the 2026 message: Just Use It! Protect yourself, your partners, and contribute to a world with fewer preventable infections.
References
- AIDS Healthcare Foundation (2026) Just Use It! AHF Celebrates International Condom Day. Available at: https://www.aidshealth.org/2026/02/just-use-it-ahf-celebrates-international-condom-day (Accessed: 13 February 2026).
- AIDS Healthcare Foundation (n.d.) AHF Celebrates International Condom Day. Available at: https://ahf.org/ahf-celebrates-international-condom-day (Accessed: 13 February 2026).
- Centers for Disease Control and Prevention (CDC) (2024) Preventing HIV with Condoms. Available at: https://www.cdc.gov/hiv/prevention/condoms.html (Accessed: 13 February 2026).
- Gov.UK University freshers urged to use condoms as STI cases remain high https://www.gov.uk/government/news/university-freshers-urged-to-use-condoms-as-sti-cases-remain-high (Accessed: 13 February 2026).
- National Day Calendar (n.d.) International Condom Day – February 13. Available at: https://www.nationaldaycalendar.com/national-day/international-condom-day-february-13 (Accessed: 13 February 2026).
- UK Health Security Agency (UKHSA) (2025) University freshers urged to use condoms as STI cases remain high. Available at: https://www.gov.uk/government/news/university-freshers-urged-to-use-condoms-as-sti-cases-remain-high (Accessed: 13 February 2026).
- World Health Organization (WHO) (2025) Condoms. Available at: https://www.who.int/news-room/fact-sheets/detail/condoms (Accessed: 13 February 2026).
- Weller, S. and Davis, K. (2002) ‘Condom effectiveness in reducing heterosexual HIV transmission’, Cochrane Database of Systematic Reviews, (1). doi: 10.1002/14651858.CD003255. (Note: Classic meta-analysis supporting ~80% reduction.)
- World Health Organization Regional Office for Europe (2024) Alarming decline in adolescent condom use. Available at: https://www.who.int/europe/news/item/29-08-2024-alarming-decline-in-adolescent-condom-use–increased-risk-of-sexually-transmitted-infections-and-unintended-pregnancies–reveals-new-who-report (Accessed: 13 February 2026).

